Summary
- Age-friendly leaders and teams can use the skill of palliative care colleagues to deliver whole-person care — supporting what matters, managing symptoms, and improving quality of life at every stage.
Palliative care is specialized care for people living with a serious illness and those who matter most to them. It treats the whole person and improves quality of life by managing symptoms, and through care planning, education, and support. Palliative care is appropriate at any age or stage of an illness. It can be provided along with all other medical treatment.
The 4Ms Framework of an Age-Friendly Health System identifies the core subjects that should drive the care of older adults. The 4Ms (What Matters, Medication, Mentation, and Mobility) align with the approach of palliative care teams and are part of their comprehensive assessment. Age-friendly leaders and team members can use the expertise of palliative care colleagues to implement the 4Ms.
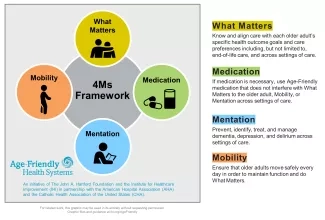
As you are providing age-friendly care, think about how you can collaborate with and learn from the palliative care team.
Scenario: Bernice’s Story
As an example, consider the hypothetical case of Bernice. Bernice is a 92-year-old widow who treasures her children and grandchildren. A former ecology teacher, she likes watching birds from her window. After a fall in her assisted living facility, Bernice was admitted to the hospital for a hip fracture. Her medical team asked palliative care to see her for pain management.
The palliative care team’s nurse practitioner, Sean, started by reviewing Bernice’s chart. This included information about previous hospitalizations, outpatient notes, and her home and hospital medications. He began to get a sense of who she is, her medical history, and how she had been doing lately. He noted that she had had a couple of recent falls and now uses a walker to safely get around (connected to one of the 4Ms, Mobility). Then he went to see her.
Starting a Conversation
Sean introduced himself as a pain management expert. (Palliative care clinicians may introduce themselves to patients by focusing on their specific symptoms and concerns.) He started by assessing Bernice’s pain. She was able to talk a little about it but wasn’t very specific. He also assessed for constipation, sleepiness, or breathing issues, because she had been taking low-dose opioid pain medications. She had trouble answering some of his questions. He also spoke with her nurse to get more details.
From that information, Sean developed recommendations for Bernice’s pain management. For instance, in addition to the opioids, she was prescribed ibuprofen for pain, which is on the Beers list of medications to avoid for older people. Instead, he recommended acetaminophen. Also, she was prescribed a stool softener, which is less effective for opioid-induced constipation than a stimulant laxative like senna. He further suggested prune juice. Bernice’s daughter had told the nurse that prune juice has worked effectively at home (Medication).
Sean also assessed Bernice’s understanding of her medical situation. She was somewhat confused and struggled to share details of her history. This seems to be a change in her mental status, based on previous clinical notes. He flagged his concern for possible delirium — sudden confusion that requires immediate medical treatment. The delirium might be caused by her pain, her opioid pain medications, depression, or simply being in the hospital. He wasn’t able to fully assess for depression because of her cognitive status. However, he spoke with her team about instituting a delirium protocol and monitoring her cognitive status. He also raised the concern that she may have previously had signs of dementia. This hospitalization might be exacerbating her cognitive issues, which can happen in older patients (Mentation).
Focusing on What Matters
Because Bernice can’t answer all his questions, Sean got her permission to call her daughter, Arlette. Arlette told him that her mother has been declining somewhat over the past few months, with increasing periods of forgetfulness.
Sean asked Arlette, “Do you know what your mother would say is most important for her health and care?” He said that this could include any of her goals and what’s important to her about each of the 4Ms. Both age-friendly care and palliative care support advance care planning, and they also focus on what matters to a person’s health and well‑being at every stage.
Arlette said they discussed this a year ago. At the time, Bernice said that what matters to her is that she be able to spend time with her family and watch her birds. Bernice also has an advance directive. It states she wouldn’t want to be put on life support or live in a nursing home. Sean wrote down what Arlette shared in Bernice’s chart. He also asked Arlette to bring the advance directive to the hospital to put in her chart. He told Bernice’s team about her preferences and her advance directive. He suggested that the team meet with Bernice and her family to discuss what matters to her in regard to treatment for her hip fracture (What Matters).
Making a Care Plan
At that meeting, the team discussed the possibility of Bernice having surgery to fix her hip and help with her pain and mobility. There were concerns about her mental status, and that surgery and anesthesia could make her delirium worse. And, her baseline cognitive status could make it hard for her to fully participate in physical therapy afterwards.
Most of the meeting focused on what mattered most to Bernice and her family. Bernice wants to be an active participant in her care decisions as much as possible. Also, she repeated that she wouldn’t want to go to a nursing home, which could be a possibility if she can’t fully participate in rehab. They all agreed to first treat the delirium through better sleep hygiene, hydration, reorienting her, and deprescribing high-risk medications. If those efforts are successful, surgery will be considered. That approach increases the likelihood that she’ll be more engaged in her recovery, which is important to her and her family. Sean and the team will be able to keep her comfortable throughout the process. If her delirium doesn’t improve, they’ll revisit her goals of care and determine the best way to support what matters to her at that point. The team is aware of Bernice’s desire to be close to her family. This will factor into her discharge options.
In caring for Bernice, Sean focused on all the 4Ms throughout the process.
Learning from Palliative Care
Having palliative care resources available for all older patients with serious illness can help address what matters and support reliable practice of the 4Ms. As the Age-Friendly Health Systems movement grows, more health systems are working to spread age-friendly care across all their sites and settings of care. Palliative care team members have deep experience with the 4Ms and can model how to use them for other clinicians in their health system. Members of the public can ask to be seen by the palliative care team if they or someone they care about is in the hospital with a serious illness. Palliative care can help provide care with all 4Ms.
Marian Grant, DNP, ACNP-BC, ACHPN, FPCN, FAAN, is a policy consultant for the Center to Advance Palliative Care (CAPC) and Chair of Maryland’s Advisory Council for Serious Illness Care.
Photo from Serious Illness Messages by Anthony Back
You may also be interested in:
- The Conversation Project’s guide for talking with your health care team about care through the end of life
- Designing Patient-Centered Health Systems for an Aging Population
- How Speech-Language Pathologists Support People to Communicate What Matters Most
