Telemedicine: Ensuring Safe, Equitable, Person-Centered Virtual Care
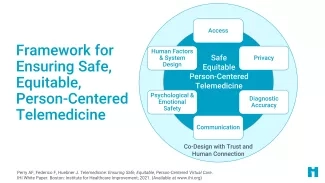
This white paper describes a framework to guide health care organizations in their efforts to provide safe, equitable, person-centered telemedicine. The framework includes six elements to consider: access, privacy, diagnostic accuracy, communication, psychological and emotional safety, and human factors and system design.
Highlights
- A framework with six elements in the context of ensuring safe, equitable, person-centered telemedicine
- Recommendations for implementing the framework elements
- The importance of co-designing telemedicine services with key stakeholders, including patients, families, and the health care workforce
- Considerations for the future of telemedicine
The COVID-19 pandemic accelerated a shift that has been slowly underway for years — the transition to telemedicine, defined as the diagnosis and treatment of patients through telecommunications technology. In the eagerness to adopt telemedicine, it is crucial to not lose sight of the key principles of quality as well as the unique risks, opportunities, and potential unintended consequences of virtual care. Health systems and providers will need guidance to successfully implement safe, high-quality telemedicine services.
In 2020, the Institute for Healthcare Improvement Lucian Leape Institute convened a panel of experts from around the world to develop a framework for telemedicine that focuses on three aspects of quality: safety, equity, and person-centeredness. The resulting framework described in the white paper includes six elements to consider:
- Access
- Privacy
- Diagnostic accuracy
- Communication
- Psychological and emotional safety
- Human factors and system design
While the paper focuses primarily on telemedicine, implications for telehealth more generally are also considered.
How to Cite This Paper:
Perry AF, Federico F, Huebner J. Telemedicine: Ensuring Safe, Equitable, Person-Centered Virtual Care. IHI White Paper. Boston: Institute for Healthcare Improvement; 2021. (Available at ihi.org)
Download Telemedicine White Paper
* Required fields
