Summary
- “Using the [Age-Friendly] 4Ms to focus the care plan on what matters to the patient is where we can make a difference in their life.”
When Laurence Solberg, MD, is asked to explain age-friendly care, he describes the experience of one patient as an example. This man, a Vietnam veteran, was in the short-term rehabilitation facility at the Community Living Center (CLC) nursing home, in the Veterans Health System in Gainesville, Florida.
Solberg asked this patient what mattered to him. He said, “No one’s ever asked me that before.” After giving it some thought, the patient said, “I’m here because I can’t do a lot for myself.” Solberg asked, “What’s the one thing that you wish you could change?” He said he was not able to use the toilet by himself. “I hate having to get cleaned up by the nurses,” he said. “It makes me feel less of a man.”
Solberg is Associate Director for Clinical Innovations at the Geriatric Research Education and Clinical Center in Gainesville, Florida, and he cares for veterans in the CLC. Before this conversation, his team’s care plan had focused on their standard definition of functioning, including helping the patient walk. After the conversation, they changed the plan to address his expressed priority. In addition to walking, therapy focused on helping the patient get up on his own and move to a bedside commode.
In four weeks, with diligent effort, he was able to do this by himself so he did not have to call a nurse. “He was able to advance in therapies so he could transfer to the toilet, and then he was able to make more progress so that he could go home,” Solberg recalls. Managing to do what was most important to him seemed to give the veteran the motivation to accomplish more than the care team had originally thought possible.
This is an example of why What Matters is at the heart of age-friendly care. The US Veterans Health Administration (VHA) is part of Age-Friendly Health Systems (AFHS), an initiative of The John A. Hartford Foundation and the Institute for Healthcare Improvement, in partnership with the American Hospital Association and the Catholic Health Association of the United States. Becoming an Age-Friendly Health System entails reliably providing a set of four evidence-based elements of high-quality care, known as the “4Ms,” to all older adults in your system: What Matters, Medication, Mentation, and Mobility.
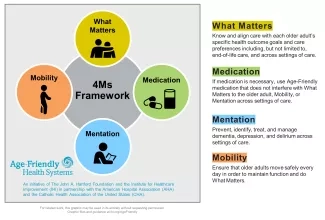
Figure 1. 4Ms Framework of an Age-Friendly Health System
Saving Time, Clarifying a Sense of Purpose
Some staff members might fear that implementing the 4Ms will merely increase their workload. But, Solberg says, that is not the case. Rather, the 4Ms offer a way to reorient care. What Matters is at the center, and the other 4Ms follow from there. For example, mobility goals will be determined based on the patient’s priorities. “If they want to be able to play with their grandchildren, but their knees hurt too much, we have to do something about that and not focus on something else that doesn’t matter to them as much,” says Solberg. “Using the 4Ms to focus the care plan on what matters to the patient is where we can make a difference in their life.”
Shaping the care plan around What Matters helps the veterans “realize what’s important to them,” says Solberg. The care team also uses the 4Ms Framework to explain to patients how goals for mobility, medications, and mentation are mobilized to achieve What Matters.
When they introduced the 4Ms Framework to the nurses, patient care aides, pharmacists, therapists, and others, Solberg and his colleagues shared examples of the 4Ms care they were already providing. “We emphasized that we were now putting the pieces together to focus on the veteran's highest priorities,” he explains.
Solberg also highlighted the importance of involving all staff members in the 4Ms work. “When everyone gave input into all the 4Ms, that’s when it didn’t come off as an edict coming down to them,” Solberg notes. “That’s when their input empowered them to be a part of this.”
The team also incorporated the 4Ms into their interdisciplinary team meeting. In these meetings, they discuss all the veterans on the unit — about 25 patients. Before incorporating the 4Ms, the meetings took two days for four hours each day. “We used to meander a bit in our discussion,” says Solberg. “We would talk about one thing and then talk about another, and then come back to the medication, talk about mobility, but then come back to medication.” When the team began structuring their meetings around the 4Ms, their patient discussions became far more efficient. They reduced the total meeting time from eight hours to two hours. “Those six hours are now given back to patient care,” says Solberg.
Advice for Others
For organizations starting out on 4Ms care, Solberg advises them to assess what they already do. It’s likely that much of their current care aligns with the 4Ms. The VHA, for example, had many programs engaged in relevant work. “We weren’t asking what matters to patients, specifically, but nurses would ask questions and get some background to learn more about the veterans as people,” says Solberg. They were also performing medication reviews. But there was no larger framework to tie it all together.
Solberg is passionate about the value of being part of the Age-Friendly community. The VHA now has more than 200 sites that are recognized as Age-Friendly. Their participation has provided “this incredible community that is open to sharing resources and experiences,” he explains. “Everyone wants to help you improve,” says Solberg. Not only has this helped his teams gain new insights and access to resources, but it has also inspired the VHA to replicate that spirit of generosity and support within their own organization. “Being able to rely on that community for backup has been a great part of the experience.”
You may also be interested in:
To have more efficient, effective, and productive appointments, share this new guide, My Health Checklist, with patients before they come in.
On April 10, 2024, the Centers for Medicare & Medicaid Services (CMS) proposed the Age-Friendly Hospital measure. It encourages hospitals to improve care for patients aged 65 years or older. You can show your support for this important measure to improve the quality of care for older adults by leaving a comment before Sunday, June 2, 2024. For more details: Age-Friendly Attestation Measure in the Federal Register.
Register for the Spring 2024 Age-Friendly Health Systems Action Community
