Why It Matters
Change is rarely easy, especially amid an exhausting pandemic. “People are burnt out at this time,” said Sadia Abbasi, MD, a physician at Stony Brook University Hospital (SBUH), a 624-bed academic medical center on Long Island, in New York State. “They don’t want to take on new initiatives.”
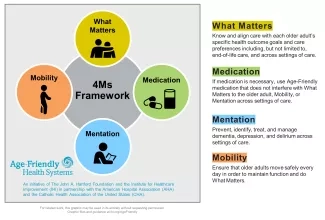
But Abbasi, an American Hospital Association (AHA) Next Generation Leaders Fellow, and her team persisted with introducing the Age-Friendly Health Systems “4Ms” Framework (Figure 1 below) on two medicine units because she and SBUH leaders knew it aligned with their mission to improve care for their patients. “About 70 percent of our population is elderly,” Abbasi noted. “This is the population we need to focus on for good outcomes.”
Understanding the reluctance to take on more work while already facing unprecedented demands, Abbasi and other Age-Friendly champions helped their colleagues see how — instead of increasing their workload — the 4Ms would help them do their current jobs more effectively. “We’re trying to tell them this is not something new,” she said. “This is something we should be doing anyway. We’re just trying to align the care with patients’ goals. We’re streamlining the workflows.”
Putting the 4Ms Into Practice
In 2019, SBUH leaders joined Age-Friendly Health Systems, an initiative of the Institute for Healthcare Improvement (IHI) and The John A. Hartford Foundation in partnership with the AHA and the Catholic Healthcare Association of the US (CHA). Joining AFHS means committing to age-friendly care, defined as evidence-based care that includes the 4Ms — What Matters, Medication, Mentation, and Mobility — causes no harm, and is grounded in What Matters to the older adult.
The following describes how Abbasi’s team incorporated the 4Ms into established care practices:
What Matters
Abbasi and her team ask older adult patients if each aspect of their care is aligned with their wishes and priorities. “While physicians have great intentions, they often forget to take into account what matters most for the patients and their families,” said Abbasi. “It is very important to align the care plan with those goals.”
To facilitate this alignment, nurses ask every newly admitted patient What Matters most to them and record it on the white boards in every patient’s room. Their answers range from wanting to be discharged, to being pain-free, to being able to attend a certain event. Then, when care providers enter the room to see the patient, they acknowledge the content on the board and discuss it with the patient.
Medication
With help from SBUH’s IT department, the Beers Criteria Medication List of potentially inappropriate medications for older adults is being incorporated into the electronic health record (EHR). Providers will receive an alert if they attempt to prescribe one of these medications. “For pain relief, what approach and medications are recommended for older patients?” said Abbasi. “What are the appropriate doses of antipsychotics for the elderly?” A new reference in the EHR includes answers to these questions.
Mentation
Abbasi and her team were aware that delirium is associated with various adverse outcomes, including longer length of stay. Therefore, their goal is to identify delirium as early as possible. At admission, a nurse assesses every older adult with the Nursing Delirium Screening Scale (NuDesc). They also conduct this assessment at the beginning or end of each shift or whenever a patient exhibits concerning signs. The nurse then notifies the physician if further assessment is needed. SBUH also offers ongoing nursing and physician education to support identifying and treating delirium.
Mobility
The team has just started implementing an early mobility program. They are engaging physical therapists, nursing, and nursing assistants to screen every patient for fall risk and promote appropriate mobility. A majority of SBUH’s older adult patients are admitted through the emergency department (ED). In the ED, they use the Morse fall scale to determine fall risk. They are also piloting the implementation of the Bedside Mobility Assessment Tool (BMAT) on certain units so that they can offer older adults appropriate support for mobility and ensure they exercise caution as needed.
Positive Responses
Although it’s too early to have solid data on outcomes, Abbasi has noted some positive developments, including the enthusiastic support of SBUH leadership. They immediately grasped that improving care for older adults was not only the right thing to do, but would have financial benefits, such as reduced length of stay.
Most importantly, older adults and their families have expressed appreciation and gratitude. They particularly welcome the policy of writing What Matters on their white boards. “What matters to me the most is being captured here,” one older adult told Abbasi. “That gives me a lot of relief and comfort. You are treating me like a human being. You are keeping my priorities in mind.”
As a result of their progress, SBUH has been recognized by AFHS as Committed to Care Excellence.
You may also be interested in:
