Summary
- A new paper describes a cross-sector partnership between the public health and health care sectors
What Matters to patients is at the heart of the Institute for Healthcare Improvement (IHI) Age-Friendly Health Systems (AFHS) initiative. This can mean prioritizing the experience of older adults when they encounter problems with services meant to help them.
For example, as part of our efforts to validate materials meant to align AFHS with public health efforts, we witnessed an exchange between an older adult and a frontline health care worker. The older adult shared her frustration with trying to navigate virtual, phone-based translation services. In contrast, the health care worker called the service a great asset for communities where providers do not speak the same language as their patients. Judging by her body language and response, the older adult clearly did not share this positive appraisal.
When debriefing about the feedback session later, we noted the conflicting assessments. We ultimately decided to give more weight to the lived experience of the older adult and highlighted her suggestions for improvement.
Bringing Age-Friendly Care to Public Health
Understanding and aligning care with each older adult’s health goals and preferences (What Matters) is an essential part of providing age-friendly care. Age-Friendly Health Systems is an initiative of The John A. Hartford Foundation and IHI, in partnership with the American Hospital Association and the Catholic Health Association of the United States. Becoming an Age-Friendly Health System entails reliably providing a set of four evidence-based elements of high-quality care, known as the “4Ms,” to all older adults in your system: What Matters, Medication, Mentation, and Mobility.
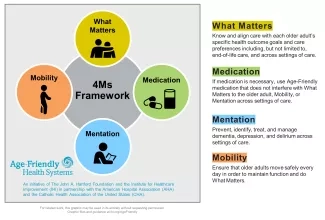
Figure 1. 4Ms Framework of an Age-Friendly Health System
The COVID-19 pandemic highlighted the need to collaborate with others to bring the age-friendly approach to public health efforts. Starting in 2021, IHI has been partnering with Trust for America’s Health (TFAH) and the Michigan Health and Hospital Association (MHA) to align Age-Friendly Health Systems with Age-Friendly public health systems. Together, we have developed the Three Keys to Cross-Sector Age-Friendly Care framework that includes an implementation guide, workbook, driver diagram (including measures and changes ideas), and care journey maps. An article published recently in Social Innovations Journal, co-authored by IHI Project Director Laura Howell Nelson, describes this cross-sector collaboration and its results.
The Three Keys are:
- What Matters
- Supportive System Structures
- Financial Structures & Policy Landscape
Drawing on the framework of upstream and downstream approaches utilized in public health, each key functions at different levels so that health disparities can be addressed through a systems approach. This means medical care is provided to individuals while simultaneously advocating for equitable policy and regulation. We developed the Three Keys through a review of the literature, an environmental scan, and most importantly by engaging those with lived experience, through key informant interviews with older adults, caregivers, and organizational leaders.
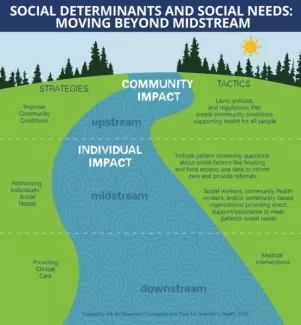
Figure 2. Source: “Health Affairs: Meeting Individual Social Needs Falls Short Of Addressing Social Determinants Of Health”
To improve the health of older adults in Michigan, the project team conducted video interviews with organizational leaders to understand and identify gaps in resources, care, and systems. Following the interviews, it was clear we needed to speak with older adults and caregivers about their experiences.
Centering the experience of older adults and hearing from them directly was vital to the success of this initiative. The MHA led the outreach effort, tapping into Family Advisory Councils (FACs) and stakeholder organizations, including a network of senior centers, to spread the word and reach a diverse group of older adults and caregivers.
In the spring of 2022, the project team conducted semi-structured qualitative interviews with 13 adults over the age of 60 or their caregivers to understand and identify care gaps and challenges for older adults over a three-month period. To obtain maximum variation in perspectives and experiences, we recruited White and BIPOC (Black, Indigenous, and people of color) residents from five Michigan cities. We obtained a diverse participant sample, with participants reporting diverse gender identities and socioeconomic statuses and 38 percent of the sample identifying as BIPOC. The majority (53 percent) self-identified as White. Interviews included participants from rural (53 percent) and urban (38 percent) communities.
For both sets of interviews, we conducted qualitative analyses to understand the impact of the current system and existing bright spots. We also asked those most affected or closest to the systems for recommendations on how to improve the system. The themes, especially those from the older adult and caregiver interviews, helped us generate the Three Keys and were key inputs into the Driver Diagram and Care Journey Maps.
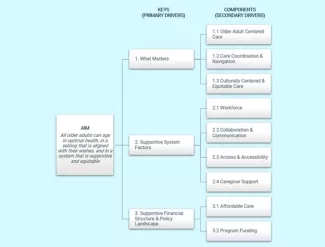
Figure 3. The Three Keys to Cross-Sector Age-Friendly Care Driver Diagram
After drafting the Driver Diagram and Care Journey Maps, the project team invited organizational leaders, older adults, and caregivers to review the materials generated from their interviews in “validation sessions.” We held two sessions in early 2023 to integrate their feedback and ensure that we centered older adults in all materials. In other words, our goal was to verify that we fully represented participants’ experiences in the core of the framework and supporting materials instead of as an aside or afterthought. Unprompted by the facilitators, one organizational leader shared that she could see What Matters to older adults throughout the framework and supporting materials.
Laura Howell Nelson is an IHI Project Director.
You may also be interested in:
On April 10, 2024, the Centers for Medicare & Medicaid Services (CMS) proposed the Age-Friendly Hospital measure. It encourages hospitals to improve care for patients aged 65 years or older. You can show your support for this important measure to improve the quality of care for older adults by leaving a comment before Monday, June 10, 2024. For more details: Age-Friendly Attestation Measure in the Federal Register.
Social Innovation Journal — “Engaging Key Stakeholders in the Development of a Framework & Toolkit for Age-Friendly Cross-Sector Care Coordination: Three Keys for Aligning the Health Care & Public Health Sectors.”
Three Keys to Cross-Sector Age-Friendly Care — includes the full set of care journey maps and driver diagram
