Why It Matters
Without industry standards for identifying health care inequities and how to measure them, it can be harder to understand best practices for closing equity gaps.
A health care executive sits down with their quality team to review quarterly performance measures and set targets for improving the equity of care across several clinical conditions. Health equity is part of the organization’s strategic plan and an increasing number of regulatory bodies are requiring data on reducing health inequities. The team engages in a thoughtful conversation about how to identify focus populations, stratify their data, and define a meaningful difference in clinical outcomes. While they reach a consensus as a local leadership team, they are uncertain if their approach conforms to best practice and wonder how other health systems measure health equity and health disparities.
The Institute for Healthcare Improvement (IHI) Leadership Alliance recently formed a Health Equity Accelerator to define an industry standard for establishing health equity measures. The Accelerator is led by an advisory group that includes Sutter Health (Sacramento, California), Providence Health (Renton, Washington), UChicago Medicine (Chicago, Illinois), all members of the Leadership Alliance with partners from Kaiser Permanente School of Medicine and the National Committee for Quality Assurance (NCQA).
The Health Equity Accelerator formed after the inaugural Centers for Medicare & Medicaid Services (CMS) Health Equity Conference in May 2023 when executives from the advisory organizations noticed variation and lack of standardization in how their respective institutions measured health inequities. Whitney Haggerson, Vice President, Health Equity and Medicaid at Providence shared, “While health equity is a strategic priority for Providence, without an industry standard for identifying health care inequities and evaluating efforts to reduce them, I worry about the burden of meeting health equity reporting requirements at the federal level and across the seven states we operate in…We have the opportunity to help policy makers shape their thinking about this important topic, reducing administrative burden and enabling benchmarking and comparative analysis across organizations.”
The Health Equity Accelerator grew to include 12 other US-based organizations, from within and outside of the Leadership Alliance. They represent a diversity of thought and health care setting, ranging from the US South to the Pacific Northwest, and from health plans and federally qualified health centers to academic medical centers and free-standing hospitals. The group seeks to define best practices across seven domains of health equity measurement: metric selection, population selection, stratification, comparison/benchmark, characterizing the inequity, confidence, and a culture of equity.
As Kristen Azar, RN, MSN/MPH, FAHA, Executive Director of the Sutter Health Institute for Advancing Health Equity explained about the selection of these domains, “We chose these domains because they are natural decision points in the measurement process. As we surveyed more and more health systems, it became clear that these were the questions that quality teams are grappling with and that the answers make a huge difference in determining which gaps are identified, prioritized for resources and ultimately closed.”

The Need for Clarity
To better understand the current state of health equity measurement, the Health Equity Accelerator began with a comprehensive review of the literature about measuring and tracking health care inequities. The review highlighted a need for clearer guidance on approaches to measurement and practical tips for stratifying, comparing, and understanding equity metrics.
The Accelerator then administered a survey to health care organizations about the seven domains of interest. Twenty-seven organizations responded, with results again demonstrating variability in how health inequities were identified and quantified.
Finally, the Health Equity Accelerator spoke to executives from the Leadership Alliance and transcribed and thematically coded roundtable discussions about health equity measurement. While many executives could articulate the importance of a culture of equity that incentivizes leaders to ameliorate health inequities and describe efforts to collect and stratify demographic data, more granular details about health equity metrics proved elusive.
With generous support from Genentech, the Health Equity Accelerator gathered at the Sutter Health Innovation Center in San Francisco, California, for a two-day retreat in March 2024. Participating organizations heard from health equity measurement subject matters experts, including Reggie Tucker-Seeley, MA, ScM, ScD, (Health Equity Strategies and Solutions); Marshall Chin, MD, MPH, (UChicago Medicine); Aswita Tan-McGrory, MBA, MSPH, (Mass General Hospital); and Megan Beckett, PhD, (RAND). Tosan Boyo, MPH, FACHE, President of Sutter Health's East Bay Market and IHI Board Member stated, “It was Sutter Health’s pleasure to host the IHI Health Equity Accelerator retreat. We look to IHI’s expertise in quality improvement science and robust network in the Leadership Alliance to join us as partners in advancing optimal health for all.”

IHI Health Equity Accelerator Group

IHI Health Equity Accelerator Group retreat presentations
During the retreat, Chin urged the Accelerator to be specific about the questions they seek to answer, clearly define the audience for the recommendations, and specify the estimated timeframe in which they could be operationalized. Tucker-Seeley reviewed his research on identifying health inequities and emphasized how measures of disparity, such as absolute and relative differences, will vary depending on the question being asked.
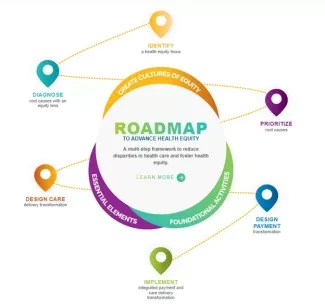
Figure 1. Advancing Health Equity (AHE) Roadmap to Advance Health Equity
On the second day of the retreat, the Accelerator team used the Advancing Health Equity – Roadmap to Health Equity (see Figure 1 above) and decided their primary goal should be giving technical guidance on the first step of the map: identifying health inequities. The Accelerator’s recommendations will allow for flexibility depending on the health care setting and will emphasize alignment with existing quality improvement programs. The measurement guidance will be particularly valuable for health care quality and equity teams and data analysts, who will produce outputs that can be operationalized by senior leadership teams, the board, and clinician leaders.

IHI Health Equity Accelerator Group discussions
In May 2024, members of the Health Equity Accelerator will present a panel discussion during the CMS Health Equity Conference titled, “Gold Standard: Aligning on Best Practice for Measuring Health Inequities and the Impact of Efforts to Reduce Them Across the US Health Care Industry.” The discussion will include preliminary recommendations and findings.
In the coming months, the Health Equity Accelerator will produce a guidance document with best practice approaches and illustrative examples of health equity metrics dashboards. We will invite entities from across the health care ecosystem to test the recommendations and give feedback. If your organization is interested in learning about the health equity measurement best practice recommendations, please contact IHI Senior Director Nikki Tennermann (ntennermann@ihi.org).
Nikki Tennermann, LICSW, MBA, is a Senior Project Director at the Institute for Healthcare Improvement. Natalie Martinez, MPH, is a Project Manager at the Institute for Healthcare Improvement.
Retreat photographs courtesy of Terry Lorant Photography
Gold photo by Jingming Pan | Unsplash
You may also be interested in:
Accepting the Challenge to Embed Equity into Patient Safety Work
