Why It Matters
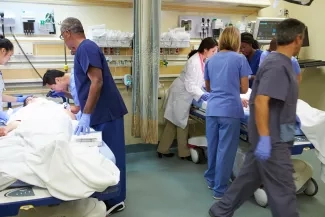
Failing to achieve hospital-wide patient flow — the right care, in the right place, at the right time — puts patients at risk for suboptimal care and potential harm. It also increases the burden on clinicians and hospital staff. IHI Senior Fellow and President Emeritus Don Berwick has said, “. . . the problem of flow is every bit as consequential for the health of our systems and the well-being of our patients” as patient safety, and deserves the same strategic prioritization.
I didn’t have to look far for a patient story to shine a spotlight on the inherent risks of inefficient care processes, mismatches of capacity and demand, and lack of timely patient progression to the appropriate care in clinical units throughout the hospital. In an informal conversation with a colleague, she shared this recollection with me:
Last year, I went to the ED at a nearby hospital because I was experiencing severe head pain, extreme vertigo, some numbness on my left side, and was rather confused. I got there around 7:00 PM, and I was seen in an exam room for the first time at around midnight. Since I suffer from migraines, they assumed that’s what was going on (although I told them repeatedly that this experience was very different from my usual episodes). My impression was that I was waiting for so long because the ED was filled with people and there were only two nurses in the ED. It was close to 4:30 AM when I finally saw a physician who said, “There’s not much we can do for you.” He said it would be best to go home and rest in my own bed since the hospital was way too crowded for me to stay. So, I went home.
I woke up the next morning at around 9:00 AM, and I felt like things were getting worse. I spoke to my friend who is a physician’s assistant at another hospital, and she told me to go back to the ED immediately to request imaging. I did. However, it was a fight to get neurological testing. Pushing and pushing, they finally agreed.
I had suffered a vertebral artery dissection and a massive blood clot had formed near the tear in the artery. As a result, I experienced a transient ischemic attack that could have resulted in a major stroke. When the doctors saw these results, they apologized for sending me home because of the overcrowding in the ED and hospital the night earlier. I was cared for in the Neuro Unit for more than a week, and it took over six months to recover.
While confirmation bias may have played a part in the doctor’s order to discharge this patient, overcrowding (and perhaps understaffing) in the ED and hospital may also have influenced the decision. This decision was clearly harmful and potentially life-threatening for the patient. Burdensome working conditions and constrained resources within the hospital may have compromised this doctor’s clinical decision-making regarding further testing and monitoring the patient’s condition.
Our patients, clinicians, and hospital staff deserve better. To address hospital-wide patient flow in hospitals, executive leaders must do the following:
- Understand the challenges and risks of poor patient flow throughout hospitals and the health system;
- Articulate why improving flow is important to hospital operations and clinical excellence;
- Integrate patient flow, safety and quality improvement goals; and
- Support and guide efforts to make system-wide improvements.
Implementing the change ideas outlined in the IHI Achieving Hospital-wide Patient Flow white paper can help your organization’s efforts to improve patient flow and patient safety. Use the white paper’s in-depth examination of a systems view of patient flow, theories for improvement, and high-leverage strategies and interventions to help your hospital and health care system reliably provide safe and timely care.
Patricia Rutherford, RN, MS, is a vice president at the Institute for Healthcare Improvement and faculty for the Hospital Flow Professional Development Program.
You may also be interested in:
IHI white paper – Achieving Hospital-wide Patient Flow
