Why It Matters
Provider organizations have expended enormous effort in the past three decades to learn and apply the principles of improvement science to clinical care. What began as a preliminary test — the National Demonstration Project launched in 1987 — has become a worldwide movement whose impact on both the quality of care and the minds of clinicians continues to spread.
However, we at IHI keep hearing a familiar litany of frustration from health care leaders: There are too many “projects” to keep up with. Hard-won improvements often backslide when the team turns its attention to other priorities. Improvement work is delegated to support specialists who are viewed with suspicion by clinical staff. Top executives just don’t “get it.”
These quality complaints are not unique to health care improvement. Joseph Juran, a colleague of Edwards Deming who was most active during the industrial quality crisis of the 1970s, maintained that achieving and sustaining quality requires a “trilogy” of complementary functions:
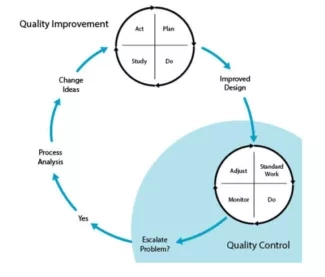
- Quality Control (QC) focuses on day-to-day operations. Sustaining reliable implementation of safe, efficient, and effective care requires that all participants — nurses, physicians, non-clinical staff, managers, everyone — maintain consistent attention to the prescribed rituals of daily work. This is where protocols and clinical evidence meet the experience of patients, and where process meets outcome. QC entails continuous critical awareness of the quality of work, and immediate, effective attention to problems large and small.
- Quality Improvement (QI) becomes necessary when stable, controlled processes are incapable of producing satisfactory results. QI involves projects that utilize the scientific method to redesign care processes to increase their safety, efficiency, effectiveness or other desirable qualities. Organizations commonly use the Model for Improvement, Lean, TQM, Six Sigma, and other methodologies for such work.
- Quality Planning (QP) refers to an overarching system for managing quality. QP comprises processes for understanding patient experience, the design of physical space, technology, standard work routines, the establishment of an open and rewarding work environment, and much more. QP also includes a system to identify gaps in performance, and commission improvement projects to close them.
In many organizations, neglect of Quality Control seems to be a root cause of many of the frustrations noted above.
In order to learn more about sustainably reliable care, an IHI R&D team in 2016 investigated management practices related to QC in 10 leading health care provider organizations. (We incorporated our findings in the IHI Sustaining Improvement white paper.) We followed that study with a pilot test of key sustainability practices in two ambulatory surgery centers in a project sponsored by AHRQ in collaboration with the Health Research & Educational Trust (HRET).
Our research and testing led us to recommend these six Quality Control practices as the most promising path to sustainability:
- Standardization denotes specific, detailed, documented standard procedures. These are not just for frontline caregivers, but also for supervisors, higher level managers, and executives. By minimizing confusion and duplication, ensuring the availability of equipment and supplies, and making sure that staff know what to do — and when and how to do it — standardization provides a stable support “platform” upon which clinicians can practice their craft. For example, to consistently and thoughtfully use surgical checklists, frontline staff must participate mindfully, every time, with the welfare of the patient as their common focus.
- Accountability means a process is in place to review implementation of standard work. The organizations we studied that have sustained best practices employ frontline huddles at the beginning of each workday or shift. Huddles maintain staff attention to standard work processes, but not just for frontline staff. The standard work of higher level managers — right up to the CEO — includes regular participation in staff huddles both as a way of monitoring and supporting care quality and reliability, and also as a demonstration of the organization’s resolve for excellence.
- Visual Management involves the use of clear, simple data displays at the unit level that show performance on key quality measures over time, and track problems the team is currently addressing. The information is posted on a board located in the workspace where the team can see it. The board provides the backdrop for huddles. In many cases, the frontline care team selects the measures to be consistent with departmental or organizational goals. The staff reviews and refreshes data daily.
- Problem Solving means methods are available for developing frontline improvement skills so staff can address issues as they arise. Consistent quality demands that frontline staff confront routine problems on a routine basis. Huddles provide a forum for raising and triaging quality problems, disposing of simple ones, and escalating more complex problems that require a formal QI project.
- Escalation involves frontline staff scoping issues and raising those that require management action to resolve. Problems that frontline staff cannot solve immediately, or that require interdepartmental coordination, are escalated to the appropriate level of management that can commission an improvement initiative. Escalation becomes part of the standard work for frontline staff and managers alike.
- Integration means active communication and consistency of purpose between levels of management and professional staff, and across departments. This is essential if the organization is to deliver on the promises made by its mission statement — for every patient, every time. Such integration requires a formal system for coordinating strategic intent with frontline quality goals, prioritizing, initiating, and managing improvement initiatives, building improvement capability, and much more.
Sustainability is ultimately the responsibility of senior leaders. Such responsibility goes beyond mission statements, marketing copy, and policy pronouncements. It also requires practical direction, support, and recognition for frontline clinical leaders — those who most directly impact patient experience of care. The standard work of senior leadership includes establishing an infrastructure for Quality Planning, and taking an active, daily role in Quality Control.
Many of IHI’s strategic partners have developed world-class improvement infrastructures and are now extending their quality work to include all three aspects of Juran’s Trilogy.
Richard Scoville, PhD, is an IHI Improvement Advisor and faculty for the Improvement Advisor Professional Development Program.
Editor’s note: For examples of specific ideas for implementing the six Quality Control practices outlined above, consult the IHI Sustaining Improvement white paper.
